Ciencias Psicológicas; v20(1)
January - June 2026
10.22235/cp.v20i1.4584
Communication
PsyCap Promotion Intervention Program (PIPP) for Healthcare Professionals: Intervention Description
Programa de intervención de promoción de PsyCap (PIPP) para profesionales de la salud: descripción de la intervención
Programa de intervenção de promoção do PsyCap (PIPP) para profissionais de saúde: descrição da intervenção
Ana Paula Pinheiro Ruiz1, ORCID 0000-0001-6215-1742
João Nuno Ribeiro Viseu2, ORCID 0000-0002-9817-7300
Cristian David Cifuentes Tinjaca3, ORCID 0000-0001-5648-2748
Saúl Neves Jesus4, ORCID 0000-0003-2019-1011
1 Universidade do Algarve, Portugal
2 Universidade de Évora, Portugal
3 Universidad Nacional de Colombia, Colombia, [email protected]
4 Universidade do Algarve, Portugal
Abstract:
The well-being of healthcare professionals is a central factor for organizational performance and sustainability and can be promoted through the development of Positive Psychological Capital (PsyCap). The main objective of this study was to describe the development methodology of the Psychological Capital Promotion Intervention Program (PIPP), its theoretical framework, and the practical description of the intervention. The development of the PIPP followed the stages of the World Health Organization’s Healthy Workplace Model, resulting in three systematic reviews and two empirical studies, culminating in the present study, which completes the planning phase. The program was designed based on the Psychological Capital Intervention (PCI), the guidelines of the Portuguese Order of Psychologists, empirical evidence, and Cognitive Behavioral Therapy (CBT) techniques. Structured into six sessions, the PIPP integrates theoretical components and practical activities, including brainstorming, SMART goal setting, role-playing, mindfulness, and cognitive restructuring, supported by eight CBT techniques. Implementation occurs in three phases, with the evaluation of effects conducted at three distinct time points. The PIPP is designed to promote the development of positive psychological resources that facilitate adaptation to challenges, goal-focused behavior, and the management of adversity, contributing to improvements in cognitive, emotional, and behavioral functioning, as well as to healthier and more productive work environments.
Keywords: health professionals; healthy workplace; intervention program; PsyCap.
Resumen:
El bienestar de los profesionales de la salud es un factor central para el desempeño y la sostenibilidad de las organizaciones, y puede promoverse mediante el desarrollo del Capital Psicológico Positivo (PsyCap). El objetivo principal de este estudio fue describir la metodología de desarrollo del Programa de Intervención para la Promoción del Capital Psicológico (PIPP), su marco teórico y la descripción práctica de la intervención. El desarrollo del PIPP siguió las etapas del Modelo de Entornos de Trabajo Saludables de la Organización Mundial de la Salud, lo que dio lugar a tres revisiones sistemáticas y dos estudios empíricos, que culminaron en el presente estudio, que completa la fase de planificación. El programa fue diseñado con base en la Intervención en Capital Psicológico (PCI), las directrices del Colegio Portugués de Psicólogos, la evidencia empírica y técnicas de la Terapia Cognitivo-Conductual (TCC). Estructurado en seis sesiones, el PIPP integra componentes teóricos y actividades prácticas, incluyendo lluvia de ideas, establecimiento de objetivos SMART, juegos de roles, mindfulness y reestructuración cognitiva, apoyadas por ocho técnicas de TCC. La implementación se desarrolla en tres fases, con la evaluación de los efectos realizada en tres momentos distintos. El PIPP está diseñado para promover el desarrollo de recursos psicológicos positivos que facilitan la adaptación a los desafíos, el enfoque en los objetivos y la gestión de la adversidad, lo que contribuye a mejoras en el funcionamiento cognitivo, emocional y conductual, así como a entornos de trabajo más saludables y productivos.
Palabras clave: lugar de trabajo saludable; profesionales de la salud; programa de intervención; PsyCap.
Resumo:
O bem-estar dos profissionais de saúde é um fator central para o desempenho e a sustentabilidade das organizações, podendo ser promovido através do desenvolvimento do Capital Psicológico Positivo (PsyCap). O objetivo geral deste estudo foi descrever a metodologia de desenvolvimento do Programa de Intervenção de Promoção do Capital Psicológico (PIPP), o seu enquadramento teórico e a descrição prática da intervenção. O desenvolvimento do PIPP seguiu as etapas do Modelo de Ambiente de Trabalho Saudável da Organização Mundial da Saúde, resultando em três revisões sistemáticas e dois estudos empíricos, culminando neste estudo, que completa a fase de “planeamento”. O programa foi concebido com base no Psychological Capital Intervention (PCI), nas orientações da Ordem dos Psicólogos Portugueses, em evidência empírica e técnicas da Terapia Cognitivo-Comportamental. Estruturado em seis sessões, o PIPP integra componentes teóricas e atividades práticas, incluindo brainstorming, definição de objetivos SMART, role-playing, mindfulness e reestruturação cognitiva, apoiadas por oito técnicas de TCC. A implementação decorre em três fases, com avaliação dos efeitos em três momentos distintos. O PIPP foi designado para promover o desenvolvimento de recursos psicológicos positivos que facilitam a adaptação aos desafios, o foco nos objetivos e a gestão da adversidade, contribuindo para melhorias no funcionamento cognitivo, emocional e comportamental, bem como para ambientes de trabalho mais saudáveis e produtivos.
Palavras-chave: ambiente de trabalho saudável; profissionais de saúde; programa de intervenção; PsyCap.
Received: 02/05/2025
Accepted: 02/02/2026
The United Nations 2030 Agenda reinforces the importance of healthy work environments and worker well-being for productivity and public health (United Nations, 2020). Well-being is a central focus of Positive Psychology (Seligman, 2012), which seeks to understand happiness and to broaden the concept of health, adaptation, creativity, and emotional fulfillment (Faria, 2020). According to the World Health Organization (WHO, 2010, 2020), employee well-being is essential for organizational competitiveness. Organizations that prioritize well-being experience greater employee retention, productivity, and sustainability, with positive impacts on performance, communities, and the global economy. It is estimated that 160 million workers develop occupational illnesses annually, and that 8% of depression cases are related to occupational hazards (WHO, 2010).
Teams are the strategic foundation of organizations (Souza et al., 2015). For teams to act effectively, it is essential that they are healthy and motivated. Among the strategies for empowering teams, Psychological Capital (PsyCap) stands out as a Positive Psychology resource that enhances motivation, resilience, and goal achievement (Luthans et al., 2007). Luthans et al. (2015) define PsyCap as a psychological state composed of self-efficacy to overcome challenges, optimism regarding present and future success, hope to pursue goals and adjust pathways when necessary, and resilience to withstand adversity and achieve success. These resources interact synergistically, influencing cognitive, affective, and behavioral functioning. Their common underlying factor is the cognitive capacity to positively evaluate situations and sustain motivated effort (Youssef-Morgan & Luthans, 2011). PsyCap is therefore considered a key resource for helping workers overcome challenges and achieve goals, offering a competitive advantage to organizations (Luthans et al., 2004; Rodrigues, 2022).
PsyCap is associated with improved performance, life satisfaction, and psychological well-being (Darvishmotevali & Ali, 2020; Kim & Yoo, 2018); and it also contributes to the creation of healthy work environments and positive workplace relationships (Caza et al., 2009). Haleem et al. (2017) highlight its relevance in professions involving direct contact with the public, as it supports the management of adversity and the adoption of behaviors that reduce stress and exhaustion. Importantly, PsyCap can be developed through targeted interventions (Luthans et al., 2006), and is recognized as a key resource for healthcare organizations seeking to promote a culture of excellence and sustainability (Caza et al., 2009).
Since its introduction, several PsyCap development interventions have been proposed. The first, the Psychological Capital Intervention (PCI), was developed by Luthans et al. (2006) and later refined by Luthans et al. (2010). Its effectiveness was subsequently confirmed in different contexts (Russo & Stoykova, 2015). Later studies further reinforced the effectiveness of PsyCap interventions, showing that PsyCap development increases positive psychological states, reduces negative states, improves well-being, and strengthens work-related coping skills (Demerouti et al., 2011; Luthans et al., 2006; Luthans et al., 2010; Luthans et al., 2014).
Despite advances in the development of PsyCap interventions, important gaps in implementation and reporting practices remain. The review conducted by Ruiz et al. (2025) identified substantial variability in intervention contexts, formats, and durations, often tailored to participants’ and organizations’ needs, and reported consistent benefits for well-being and performance, particularly in emotionally demanding contexts. However, the authors highlighted a common limitation: the lack of clear and standardized descriptions of session content, which hampers replication and standardization across programs. Converging evidence was reported by Salanova and Ortega-Maldonado (2019), whose integrative review showed that PsyCap interventions generally increase PsyCap and improve outcomes such as performance, work attitudes, and well-being, with effects sustained over time. Nevertheless, recurring weaknesses were identified, including methodological limitations, wide variability in follow-up periods, and the predominance of studies conducted in Western contexts, underscoring the need for more rigorously structured and transparently reported interventions.
To address these gaps, the present study proposes the PsyCap Promotion Intervention Program (PIPP), an intervention grounded in validated theoretical models and empirically supported techniques, offering a clearly defined and structured approach to the systematic development of PsyCap. In their review, Ruiz et al. (2025) further highlighted that Youssef-Morgan and Sundermann (2014) defined four essential criteria for effective PsyCap interventions: (1) generate outcomes attributable to the intervention, (2) modify adaptive characteristics, (3) outperform conventional programs, and (4) ensure a positive return on investment. The review found that only the first two criteria were met, underscoring the need for interventions that fulfill all four criteria (Ruiz et al., 2025). The general objective of this study was to describe the PIPP development methodology, as well as to present a theoretical and practical synthesis of its structure. The specific objectives of this study are to: (1) describe the objectives and target audience of the PIPP, (2) outline the pedagogical and operational guidelines for trainers, (3) describe the program’s ethical considerations and potential risks, (4) describe the content delivery methods, (5) present the theoretical model underpinning the PIPP, (6) describe the program structure and sessions, and (7) outline the program’s implementation and evaluation plan.
This manuscript reports the development and description of an intervention, presenting its conceptual framework, design, and implementation protocol, without reporting results from its implementation, which will be examined in a subsequent empirical study. The reporting of the intervention development was guided by the Guidance for Reporting Intervention Development Studies (GUIDED) checklist (Duncan et al., 2020).
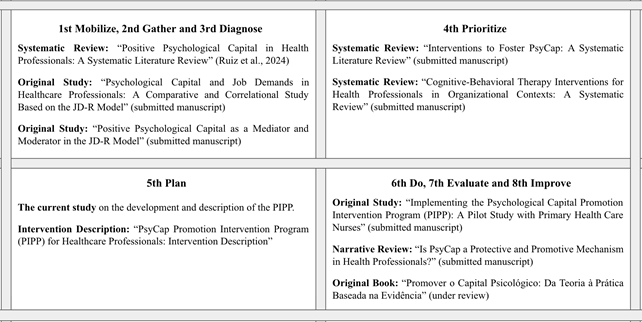
The development of the PIPP was evidence- and theory-based and guided by the World Health Organization Healthy Workplace Model, which provides a comprehensive and adaptable framework for planning, implementing, and evaluating workplace interventions, with an emphasis on continuous improvement. This model comprises eight sequential steps: mobilize, gather, diagnose, prioritize, plan, implement, evaluate, and improve (WHO, 2010). The execution of these steps resulted in a structured program of research, including three systematic reviews and two empirical studies that informed the theoretical, empirical, and methodological foundations of the PIPP. As illustrated in Figure 1, this process not only supported the planning and development of the intervention described in the present study but also gave rise to subsequent research outputs, situating the PIPP within a coherent and cumulative research framework.
Figure 1: PIPP Structuring Steps based on the World Health Organization Healthy Model
Description of the Intervention
Objective and Target Audience
The PIPP aims to promote and develop the PsyCap of health professionals in public and private organizations by enhancing self-efficacy, optimism, hope, and resilience. Furthermore, the program was designed with a structure that includes: (1) three distinct points of effectiveness evaluation, (2) cost–benefit analysis, including return on investment (ROI) and cost indicators such as presenteeism, and (3) a systematized methodology that ensures replicability across different contexts.
This program is based on the premise that strengthening individual PsyCap may contribute to the development of group PsyCap, which reflects the shared psychological state of teams and emerges from interaction and communication among members. The greater the interaction, the stronger the group’s psychological components (Santos, 2021). Bogler and Somech (2019) reinforce this view by stating that teams operating in shared contexts tend to develop shared mental models. Nunes’ perspective (Nunes, 2017) was also considered, which emphasizes that health work contexts are privileged spaces for continuous training. Thus, the PIPP aims not only to develop PsyCap but also to facilitate the practical application of the knowledge acquired in professionals’ daily work routines.
When implementing the PIPP for different professional groups, it is recommended to separate participants according to their professions, considering distinct responsibilities and challenges (Yang et al., 2020). This personalization enhances the relevance, effectiveness, and perceived benefits of the PIPP for participants.
Theoretical and Conceptual Framework: JD-R and Psychological Capital in Healthcare Organizations
The JD-R model, proposed by Demerouti et al. (2001), has become one of the leading frameworks in occupational health psychology and human resource management. It is widely applied across organizations and supported by extensive empirical evidence (Ahmed et al., 2021; Bakker & Demerouti, 2017). Its main contribution lies in its comprehensive approach, integrating job demands and job resources rather than focusing exclusively on risk and stress. Initially developed to explain emotional exhaustion, the model has evolved into a flexible framework that accounts for employee well-being, work engagement, and performance (Bakker & Demerouti, 2007, 2014; Bakker et al., 2023). Over time, this model has been consolidated as a theory through a set of core theoretical assumptions, currently comprising nine premises: flexibility, dual processes, job demands–job resources interactions, personal resources, resources moderation, job crafting, gain cycles, self-undermining, and loss cycles (Bakker et al., 2023). Within this framework, PsyCap is embedded in the fourth premise, which conceptualizes personal resources as positive self-beliefs or self-evaluations linked to individuals’ perceived control over, and impact on, their work environment (Bakker et al., 2023).
The JD-R theory not only explains occupational well-being processes but also informs the development of evidence-based workplace interventions. Grounded in the assumption that employees play an active role in shaping their work environment and that organizations should invest in their development to strengthen personal resources, the JD-R framework emphasizes interventions that support adaptation to job demands and foster professional growth (Bakker & Demerouti, 2014). Accordingly, PsyCap represents a particularly suitable construct for operationalizing the JD-R resource-based intervention pathway at the psychological level. JD-R–based interventions are typically grouped into four main categories—job redesign, job crafting, training, and strengths-based approaches—differing in level (individual vs. organizational) and intervention target (work conditions vs. personal resources; Bakker & Demerouti, 2014). Within this framework, the PIPP fits as an intervention aimed at strengthening personal resources, combining strengths-based approaches at the individual level with training at the organizational level (Bakker et al., 2023). Although not originally defined as a distinct JD-R intervention category, the PIPP can be understood as a practical application of the JD-R model, particularly in promoting personal resources.
Considering the framework proposed by the JD-R model, strengthening individual psychological resources within organizational contexts plays a central role in work adaptation and the protection of mental health, particularly when such contexts are characterized by high demands and structural changes over which employees have little control (Almeida, 2014; Chintalapti, 2021). Healthcare professionals operate in organizational contexts marked by high emotional demands, time pressure, ethical responsibility, and continuous exposure to human suffering—factors that significantly increase vulnerability to stress, emotional exhaustion, and other psychosocial risks (Almeida et al., 2020; Izdebski et al., 2023). These risks stem from organizational, managerial, and psychosocial working conditions and negatively affect both the physical and mental health of professionals, as well as the functioning and productivity of healthcare organizations (Almeida et al., 2020; Claudino et al., 2024). Evidence indicates that work environments characterized by high workloads and adverse conditions are associated with poorer performance, lower work engagement, higher turnover, increased absenteeism, and compromised quality of care, thereby threatening the sustainability of healthcare systems (Secosan et al., 2021).
Within this context, the PsyCap, composed of four core psychological capacities—hope, efficacy, resilience, and optimism—commonly referred to by the acronym HERO, stands out as a trainable psychological resource that goes beyond individuals’ current functioning, also reflecting their potential for development (Luthans et al., 2006). Professionals with higher levels of PsyCap tend to interpret job demands more positively, perceive greater control over situations, and respond more effectively to challenging environments, thereby reducing the risk of stress and emotional exhaustion (An et al., 2020; Santos et al., 2019). In the healthcare sector, higher levels of PsyCap have been associated with greater work engagement, better performance, enhanced well-being, and stronger intentions to remain in the organization, contributing to healthier and more sustainable work environments (Lupșa et al., 2020; Secosan et al., 2021; Viseu, 2017). Therefore, interventions aimed at developing PsyCap are particularly suitable for healthcare organizational contexts, especially when implemented in a structured manner, with organizational support and under conditions that foster participation, psychological reflection, and the practical application of the skills developed.
Theoretical Model of the PIPP and Associated Theories
The development of the PIPP followed the guidelines of the Portuguese Order of Psychologists (OPP), adapting recommendations for preventive interventions to a skills development program. These guidelines recommend that programs be grounded in empirically validated theoretical models, ensuring consistency between objectives, processes, and outcomes (Matos, 2017). The theoretical model underlying the PIPP is based on the definition of PsyCap proposed by Luthans et al. (2015) and on the PCI framework (Luthans et al., 2006; Figure 2).
The PCI was developed in 2006 as an online micro-intervention consisting of two-hour workshops. The authors administered the Psychological Capital Questionnaire (PCQ-24; Luthans et al., 2007) and found a significant increase in PsyCap. In 2010, the intervention was replicated, yielding similarly positive effects (Luthans et al., 2010). The intervention guidelines were based on the PsyCap dimensions and grounded in clinical psychology (hope and resilience), attribution and expectancy theories (optimism), and Bandura’s theory (self-efficacy; Bandura, 1997). Each dimension was developed through specific exercises: (1) hope: goal focus and a proactive mindset, (2) self-efficacy: goal setting and positive feedback, (3) resilience: anticipating obstacles, and (4) optimism: reframing negative thoughts. These exercises were followed by writing, reflection, and group discussion activities, as well as the formulation of personal goals and strategies to overcome potential barriers. The results confirmed that developing PsyCap provides a competitive advantage and improves job performance (Luthans et al., 2006; Luthans et al., 2010).
Figure 2: PsyCap Intervention (PCI)
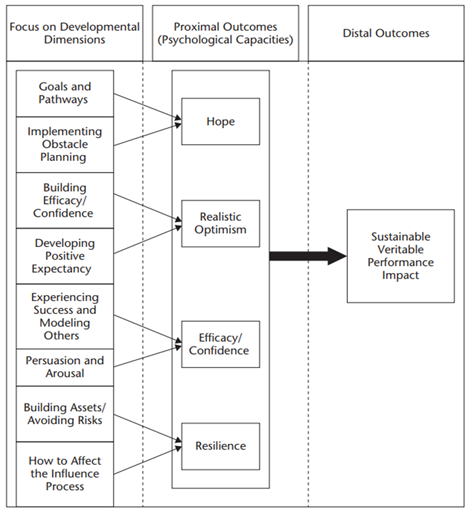
Note: Prepared by the authors based on the model by Luthans et al. (2006).
This theoretical grounding in the PCI was corroborated by the review conducted by Ruiz et al. (2025), which found that 81.81 % of the analyzed articles used it as a theoretical anchor. Within this model, each PsyCap component is supported by specific theories: hope, by Snyder et al.’s Theory of Hope (Snyder et al., 1991); self-efficacy, by Bandura’s social cognitive theory; resilience, by Ann Masten’s work in positive psychology; and optimism, as conceptualized by Youssef-Morgan and Luthans (2011) within the field of positive psychology. The theoretical definitions of each resource were used to structure the practical activities.
Russo and Stoykova (2015) followed the PCI guidelines and implemented an intervention consisting of four exercises: (1) defining Specific, Measurable, Attainable, Relevant and Time-bounded (SMART) goals (hope), (2) identifying realistic goals and obstacles (hope and self-efficacy), (3) establishing subgoals (resilience), and (4) recognizing individual and contextual resources (resilience). In addition, the intervention included a constructive feedback activity and small-group brainstorming sessions (four to five participants) focused on positive thinking (self-efficacy and optimism). The PCQ-24 (Luthans et al., 2007) was administered at three time points: before the intervention, immediately after, and one month later.
As with the PCI, the PIPP sessions were structured to develop each PsyCap component separately. The selected activities are empirically supported, drawing on evidence from the PCI, the study by (Russo & Stoykova, 2015), and the review by Ruiz et al. (2025), which identified effective content delivery methods such as structured reading materials, positive feedback techniques, goal setting and achievement, PowerPoint presentations, videos, mindfulness, and practical exercises. The review also considered specific empirical studies, including Gon et al. (2023), conducted with nurses, and Zeng et al. (2023), which incorporated mindfulness and reported benefits for self-efficacy, hope, and resilience.
Consistent with its theoretical foundations, the PIPP adopts a content delivery approach that integrates theoretical exposition (oral presentations) with participatory techniques, such as role-playing, to promote active interaction between trainers and participants (Matos, 2017; Nunes, 2017). In line with PsyCap development principles, the program also incorporates experience-based learning strategies, including guided reflection on lived experiences (Bonvalot, 1991) and vicarious learning through observation and group exchange (Russo & Stoykova, 2015).
In addition, the activities were informed by Cognitive Behavioral Therapy (CBT) techniques selected according to the theoretical foundations of each PsyCap resource and drawn from the book 101 CBT Techniques (Conceição & Bueno, 2020). In total, eight techniques were selected: Wheel of Life (Sachweh & Conceição, 2020), Making Decisions (Nepomuceno & Conceição, 2020), Rational–Emotional Role-Play (Rudey & Conceição, 2020), Relaxation (Karvat & Conceição, 2020), One Minute Meditation (Rodrigues & Conceição, 2020), Reformulation of Mental Images (Paulitisky & Conceição, 2020), Gratitude Box (Conceição, 2020), and Criticism Circle (Hiera & Conceição, 2020). To integrate the theoretical foundations of PsyCap with the structure and objectives of the PIPP, a logic model was developed (Figure 3).
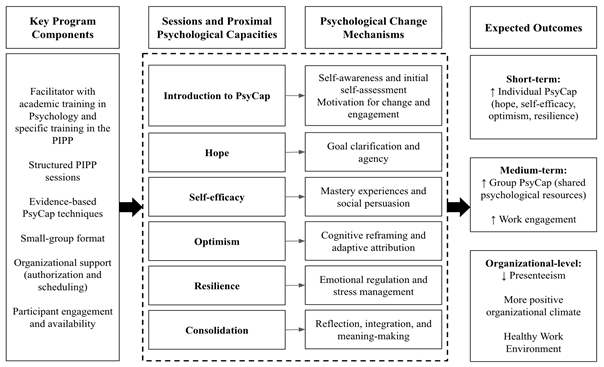
Figure 3: Logic model of the PsyCap Promotion Intervention Program (PIPP)
Note: This model synthesizes the theoretical rationale of the intervention by illustrating the hypothesized relationships among key program components, session content, proximal psychological mechanisms, and expected outcomes at the individual, group, and organizational levels.
Theoretical Anchoring and Session Description
Based on the PCI and the review by Ruiz et al. (2025), it was found that PsyCap components can be addressed in individual sessions. The review identified an average of five sessions; however, the PIPP was structured into six sessions by including an introductory session and a consolidation session (Table 1). The review also indicated that sessions lasted an average of 77 minutes and that the intervention spanned a total of six weeks (Ruiz et al., 2025).
Table 1: Description of PIPP Sessions
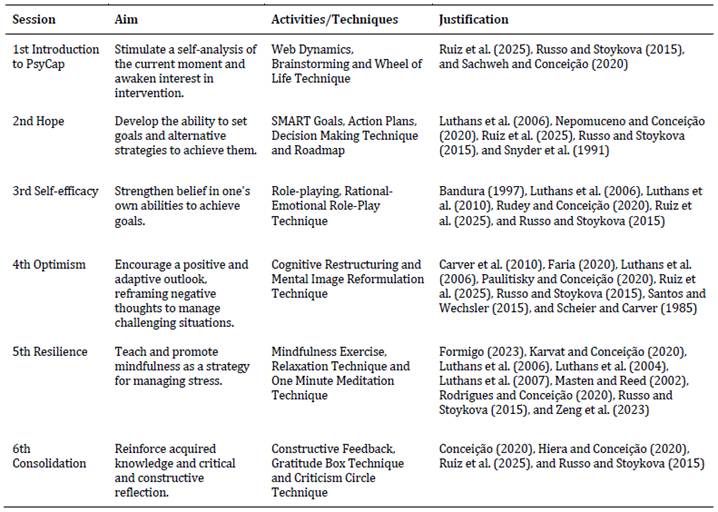
In the PIPP, sessions are planned to occur weekly, with a duration of 60 to 90 minutes, and are designed to be delivered in a mixed method format. Intervention sessions are conducted in person, whereas assessment procedures and session summaries are delivered online. Each session is held in small groups (four to five participants), encouraging attention and active listening (Russo & Stoykova, 2015). The program targets health professionals working in public or private healthcare organizations. Inclusion criteria include active professional practice in a healthcare setting and availability to attend the scheduled sessions. Exclusion criteria are limited to professionals not currently working in healthcare contexts or individuals unable to participate in group-based activities at the time of implementation.
Sessions are delivered in small groups to promote interaction, social support, experience sharing, and vicarious learning, while also being time- and cost-efficient. However, this format presents challenges, such as managing time to accommodate all groups and respond to individual needs (Nunes, 2017), making the presence of psychologists essential.
Guiding Guidelines for Trainers
We recommend carefully reading the book Promover o Capital Psicológico: Da Teoria à Prática Baseada na Evidência, which details the step-by-step implementation of the PIPP. The book includes a participant manual divided into six sections corresponding to the program sessions. It will be available for purchase and can also be requested via email ([email protected]). The implementation of the PIPP should follow the structure presented in the book, ensuring that all program components are systematically addressed. This approach maximizes the program’s impact and facilitates the monitoring and evaluation of outcomes. Moreover, this structured framework reinforces transparency and the responsibility of each trainer to deliver the program as intended.
This book was developed considering several factors that influence the effectiveness of the PIPP, including participant individuality (motivation, skills, and prior knowledge), program structure (methods, environment, and duration), and trainer profile (competence, experience, and mastery of content). To address these factors, detailed support materials are provided to guide and prepare trainers, ensuring an efficient and well-organized implementation. This emphasis is particularly important, as a well-prepared trainer can significantly enhance participant engagement (Nunes, 2017).
Ethical Considerations and Potential Risks
Ethics are fundamental in intervention programs. Although there is no specific ethical code governing this type of intervention, Nunes (2017) highlights a set of guidelines whose application depends largely on the trainer. Accordingly, trainers must hold a degree in Psychology (given the theoretical foundations of the PIPP), adopt an ethical stance, and clearly present their qualifications and the program’s objectives without making promises regarding outcomes. Although the PIPP is implemented in a group format and employs psychological techniques, it does not constitute a clinical group therapy intervention, nor does it aim to treat psychological disorders or mental pathologies. The PIPP was designed as a structured preventive and developmental intervention focused on the promotion of individual competencies and the strengthening of trainable positive psychological capacities. Rather than functioning as a therapeutic setting, it serves as a space for sharing and developing skills, free from judgment or imposed change (Nunes, 2017).
If the program evaluation is conducted as a research project, it is essential to adhere to additional ethical principles, namely compliance with the Declaration of Helsinki. The implementation of the PIPP is expected to lead to a more productive and positive work environment; however, challenges may arise, such as initial resistance and variability in effectiveness among participants. These differences may depend on factors such as openness to the change process, pre-existing stress levels, and the dynamics of the groups in which the program is implemented.
Program Application (Evaluation Phases and Moments)
The PIPP was structured to be applied in three distinct phases (Table 2).
Table 2: PIPP Application Phases
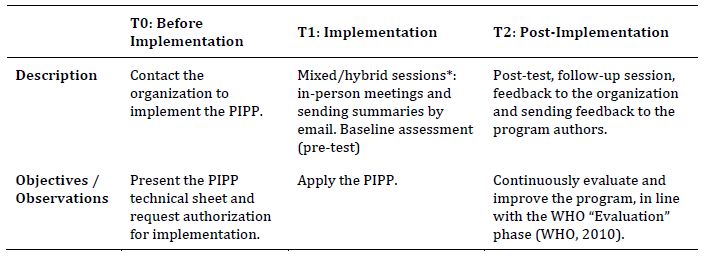
Note: *According to Carter and Youssef-Morgan (2022), there are no clear advantages to fully online interventions, which justifies the choice of a hybrid/mixed approach to increase the effectiveness of the intervention.
PIPP assessments involve the application of the same protocol across three distinct phases (pre-test, post-test, and follow-up), using validated instruments to psychometrically measure the variables under study. Trainers are responsible for authorizing and purchasing the questionnaires. Assessments should be conducted online using platforms such as Google Forms or EuSurvey, except in cases where participants experience difficulties accessing the online protocol. From an evaluation design perspective, the PIPP is conceived as a structured intervention that can be assessed using a pre-test–post-test design with follow-up measurements. Depending on the objectives, context, and resources of each implementation, evaluation designs may range from single-group longitudinal assessments to quasi-experimental or experimental designs that include control groups and randomization. When feasible, the inclusion of comparison or control groups is recommended to strengthen causal inference. Statistical analyses may include within-group comparisons across assessment time points (pre-test, post-test, and follow-up), as well as between-group analyses in designs involving experimental and control groups. Decisions regarding randomization, sample allocation, and longitudinal follow-up should be aligned with the specific research or practice goals of each implementation, as well as with ethical and organizational constraints.
Each assessment point is designed to capture different aspects of change across the intervention process and involves specific procedures and measurement instruments. Pre-testing is essential for identifying baseline PsyCap levels (and other variables) prior to the intervention and is administered during the first session. The recommended instrument is the PCQ-24 (Luthans et al., 2007), using the validated version appropriate to the country in which the program is implemented. This instrument was adopted in 80 % of the studies in Ruiz et al. (2025) due to its validity, reliability, and internal consistency (α = .89 to .93; Ruiz et al., 2024), as well as reverse scoring that reduces common method bias (Sharp, 2019). The assessment may be complemented with additional instruments, such as the Utrecht Work Engagement Scale (UWES-9; Schaufeli & Bakker, 2003).
It should be noted that extensive assessment protocols may lead to participant fatigue. Therefore, when additional questionnaires are included, the use of twelve-item versions is recommended, such as the Compound Psychological Capital Scale (CPC-12; Lorenz et al., 2016); or the revised Compound PsyCap Scale (CPC-12-R; Dudasova et al., 2021). The application of a PsyCap measurement instrument is mandatory, as without an adequate baseline assessment it is not possible to accurately evaluate the effectiveness of the intervention (Matos, 2017). Data analysis must be conducted rigorously, ensuring participant confidentiality and the ethical use of information to assess the program’s impact.
The post-test should be conducted during the sixth session or on the following day, using the same assessment protocol to measure the program’s immediate impact. Follow-up assessment should take place between 15 and 60 days after the sixth session, depending on organizational availability. This phase includes a reapplication of the protocol and a semi-structured interview, conducted either in person or online. The interview questions are provided in the PIPP book. This reassessment interval aims to capture longer-term behavioral and psychological changes and is consistent with the findings reported by Ruiz et al. (2025), who identified an average follow-up period of approximately seven weeks after the post-test. It also aligns with recommendations from Lally et al. (2010), and Stratman and Youssef-Morgan (2019), which suggest that a period of 21 to 66 days is appropriate for observing meaningful behavioral change.
These assessment points are essential for verifying the first three criteria proposed by Youssef-Morgan and Sundermann (2014). The fourth criterion can be addressed through the analysis of presenteeism and/or the calculation of return on investment (ROI; Martin et al., 2009; Read, 2024). Presenteeism can be assessed using different methods, including validated instruments such as the Stanford Presenteeism Scale (SPS-6; Koopman et al., 2002), by comparing scores across assessment periods. ROI assessment requires the identification of all relevant costs (e.g., development, training, operation, and maintenance) and the analysis of associated benefits. ROI is calculated using a standard formula and expressed as a percentage, where positive values indicate a net benefit and negative values indicate a loss. In the context of the PIPP, costs may correspond to the number of hours professionals are absent from work during program participation. When the trainer is internal and no confidentiality conflicts exist, it is also recommended to include absenteeism as a cost indicator. Figure 4 presents the planned timeline for the PIPP.
Figure 4: PIPP Program Application Schedule
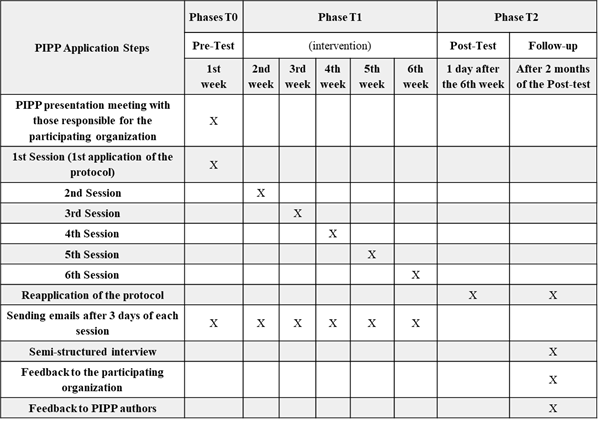
Final Considerations
The development of structured intervention programs aimed at healthcare professionals has the potential to generate meaningful benefits at both individual and organizational levels. The PIPP was designed to promote positive psychological development by strengthening core components of PsyCap, namely self-efficacy, hope, optimism, and resilience. Through the integrated development of these psychological resources, the program is expected to support adaptive cognitive, emotional, and behavioral functioning, particularly in demanding and high-pressure work contexts.
Beyond its promotive focus, the PIPP is conceptually aligned with preventive approaches to occupational stress and emotional exhaustion. By enhancing PsyCap, healthcare professionals may become better equipped to proactively manage work-related demands and psychological strain, thereby potentially reducing vulnerability to mental health problems. At the managerial level, higher PsyCap may contribute to more adaptive coping and leadership behaviors, as well as to the fostering of a more positive organizational climate, which in turn can support engagement, well-being, and sustainable work performance. However, these expected outcomes should be interpreted as theoretically grounded projections rather than empirically confirmed causal effects.
Importantly, the effectiveness of the PIPP depends on participants’ active engagement and the consistent application of the strategies and techniques developed during the sessions. Without the integration of these skills into daily professional practice, sustained gains in PsyCap are unlikely. Moreover, the program may be less effective under certain conditions, such as extreme workloads, insufficient organizational support, misalignment with organizational culture, or limited managerial endorsement. These contextual and organizational factors should be carefully considered when planning and implementing the intervention.
A key limitation of the present work is that the PIPP was not evaluated in this article through controlled effectiveness studies. However, it is important to note that the development of this intervention led to its implementation in a real-world context, carried out as part of an effectiveness study conducted with primary healthcare professionals in Portugal, the results of which will be reported in a future publication. Beyond this study, further effectiveness and implementation research is recommended, to be conducted by other authors across different organizational and cultural contexts. Such studies will allow the examination of the generalizability of the PIPP’s effects and the comparison of outcomes across contexts, populations, and implementation strategies, contributing to its refinement and external validation. Future research should examine within-group changes over time and between-group differences, as well as identify mechanisms of change and contextual moderators. Hybrid effectiveness–implementation studies may be particularly useful to understand not only whether the PIPP is effective, but also how, for whom, and under which organizational conditions it produces the best outcomes.
Overall, the PIPP represents a theoretically grounded and structured intervention proposal for the development of PsyCap in healthcare contexts. Its adaptability allows for application across different professional groups and organizational settings, provided that its core structure, session sequence, and objectives are preserved. Empirical evaluation therefore represents the next critical step to substantiate its proposed benefits and inform future refinements of the program.
References:
Ahmed, F., Zhao, F., Faraz, N. A., & Qin, Y. J. (2021). How inclusive leadership paves way for psychological well‐being of employees during trauma and crisis: A three‐wave longitudinal mediation study. Journal of Advanced Nursing, 77(2), 819-831. https://doi.org/10.1111/jan.14637
Almeida, P. D. (2014). Resistência à mudança organizacional: estudo comparativo entre os fatores que motivam a resistência à mudança organizacional em uma empresa pública e outra privada (Monografia de especialização, Universidade Tecnológica Federal do Paraná). Universidade Tecnológica Federal do Paraná https://riut.utfpr.edu.br/jspui/bitstream/1/22993/3/PB_GP_lV_2014_12.pdf
Almeida, T. C. D., Heitor, M. J., Santos, O., Costa, A., Virgolino, A., Rasga, C., Martiniano, H. & Vicente, A. (2020). Saúde mental em tempos de pandemia-SM-COVID-19: relatório final. Instituto Nacional de Saúde Doutor Ricardo Jorge, IP. http://hdl.handle.net/10400.18/7245
An, M., Shin, E. S., Choi, M. Y., Lee, Y., Hwang, Y. Y., & Kim, M. (2020). Positive psychological capital mediates the association between burnout and nursing performance outcomes among hospital nurses. International Journal of Environmental Research and Public Health, 17(16), 5988. https://doi.org/10.3390/ijerph17165988
Bakker, A. B., & Demerouti, E. (2007). The job demands‐resources model: State of the art. Journal of Managerial Psychology, 22(3), 309-328. https://doi.org/10.1108/02683940710733115
Bakker, A. B., & Demerouti, E. (2014). Job demands-resources theory. In P. Y. Chen & C. L. Cooper (Eds.), Work and wellbeing (pp. 37-64). Wiley Blackwell. https://doi.org/10.1002/9781118539415.wbwell019
Bakker, A. B., & Demerouti, E. (2017). Job demands–resources theory: Taking stock and looking forward. Journal of Occupational Health Psychology, 22(3), 273-285. https://doi.org/10.1037/ocp0000056
Bakker, A. B., Demerouti, E., & Sanz-Vergel, A. (2023). Job demands–resources theory: Ten years later. Annual Review of Organizational Psychology and Organizational Behavior, 10(1), 25-53. https://doi.org/10.1146/annurev-orgpsych-120920-053933
Bandura, A. (1997). Self-efficacy: The exercise of control. Freeman.
Bogler, R., & Somech, A. (2019). Psychological capital, team resources and organizational citizenship behavior. The Journal of Psychology, 153(8), 784-802. https://doi.org/10.1080/00223980.2019.1614515
Bonvalot, G. (1991). Éléments d’une définition de la formation expérientielle. In M. Lamoureux (Ed.), La formation expérientielle des adultes (pp. 317–325). La Documentation française.
Carter, J. W., & Youssef-Morgan, C. M. (2022). Psychological capital development effectiveness of face-to-face, online, and micro-learning interventions. Education and Information Technologies, 27(5), 6553-6575. https://doi.org/10.1007/s10639-021-10824-5
Carver, C. S., Scheier, M. F., & Segerstrom, S. C. (2010). Optimism. Clinical Psychology Review, 30(7), 879-889. https://doi.org/10.1016/j.cpr.2010.01.006
Caza, A., McCarter, M., Hargrove, D., & Was, S. (2009). Third-party effects of psychological capital: Observer attributions and responses. Academy of Management Proceedings, 2009(1), 1-6. https://doi.org/10.5465/ambpp.2009.44265238
Chintalapti, N. R. (2021). Impact of employee motivation on work performance. Anusandhan–Ndim’s Journal of Business and Management Research, 3(2), 24-33. https://doi.org/10.56411/anusandhan.2021.v3i2.24-33
Claudino, M., Pinote, S., & Manzano, M. (2024). Avaliação dos Fatores de Risco Psicossociais em Profissionais de Saúde num Centro Hospitalar Central. Revista Portuguesa de Saúde Ocupacional Online, 17, esub0429. 10.31252/RPSO.10.02.2024
Conceição, J. (2020). Técnica 101: Caixa da Gratidão. In J. Conceição & G. Bueno (Eds.), 101 técnicas da terapia cognitivo-comportamental (p. 169). UNC.
Conceição, J., & Bueno, G. (2020). 101 técnicas da terapia cognitivo-comportamental. UNC.
Darvishmotevali, M., & Ali, F. (2020). Job insecurity, subjective well-being and job performance: The moderating role of psychological capital. International Journal of Hospitality Management, 87, 102462. https://doi.org/10.1016/j.ijhm.2020.102462
Demerouti, E., Bakker, A. B., Nachreiner, F., & Schaufeli, W. B. (2001). The job demands-resources model of burnout. Journal of Applied Psychology, 86(3), 499-512. https://doi.org/10.1037/0021-9010.86.3.499
Demerouti, E., van Eeuwijk, E., Snelder, M., & Wild, U. (2011). Assessing the effects of a “personal effectiveness” training on psychological capital, assertiveness and self‐awareness using self‐other agreement. Career Development International, 16(1), 60-81. https://doi.org/10.1108/13620431111107810
Dudasova, L., Prochazka, J., Vaculik, M., & Lorenz, T. (2021). Measuring psychological capital: Revision of the compound psychological capital scale (CPC-12). PLOS ONE, 16(3), e0247114. https://doi.org/10.1371/journal.pone.0247114
Duncan, E., O'Cathain, A., Rousseau, N., Croot, L., Sworn, K., Turner, K. M., Yardley, L., & Hoddinott, P. (2020). Guidance for reporting intervention development studies in health research (GUIDED): an evidence-based consensus study. BMJ Open, 10(4), e033516. https://doi.org/10.1136/bmjopen-2019-033516
Faria, M. C. (2020, January 30th -February 1st). Contributos da psicologia positiva para a saúde e bem-estar. Actas do 13º Congresso Nacional de Psicologia da Saúde (pp. 285-293). ISPA. https://repositorio.ispa.pt/bitstream/10400.12/7529/1/13CongNacSaude_285.pdf
Formigo, J. C. F. (2023). Influência do conflito trabalho-família no desempenho individual: O papel moderador do capital psicológico positivo (Master's thesis , Instituto Superior de Gestão). Repositório Comum. http://hdl.handle.net/10400.26/46129
Gon, R., Wu, Y., Liu, Y., Yang, R., Zhang, Y., & Xing, L. (2023). Influence of group training based on psychological capital theory on nursing staff’s occupational benefits and job satisfaction in an infusion preparation center. Alternative Therapies in Health & Medicine, 29(3).
Haleem, M., Masood, S., Aziz, M., & Jami, H. (2017). Psychological capital and mental health of rescue workers. Pakistan Journal of Psychological Research, 32(2), 389-405.
Hiera, G. D., & Conceição, J. (2020). Técnica 43: Exposição e Experimento - Círculo da Crítica. In J. Conceição & G. Bueno (Eds.), 101 técnicas da terapia cognitivo-comportamental (p. 84). UNC.
Izdebski, Z., Kozakiewicz, A., Białorudzki, M., Dec-Pietrowska, J., & Mazur, J. (2023). Occupational burnout in healthcare workers, stress and other symptoms of work overload during the COVID-19 pandemic in Poland. International Journal of Environmental Research and Public Health, 20(3), 2428. https://doi.org/10.3390/ijerph20032428
Karvat, M. E., & Conceição, J. (2020). Técnica 74: Relaxamento. In J. Conceição & G. Bueno (Eds.), 101 técnicas da terapia cognitivo-comportamental (p. 127). UNC.
Kim, K. J., & Yoo, M. S. (2018). The influence of psychological capital and work engagement on intention to remain of new graduate nurses. JONA: The Journal of Nursing Administration, 48(9), 459-465. https://doi.org/10.1097/NNA.0000000000000649
Koopman, C., Pelletier, K. R., Murray, J. F., Sharda, C. E., Berger, M. L., Turpin, R. S., Hackleman, P., Gibson, P., Holmes, D., & Bendel, T. (2002). Stanford presenteeism scale: Health status and employee productivity. Journal of Occupational and Environmental Medicine, 44(1), 14-20. https://doi.org/10.1097/00043764-200201000-00004
Lally, P., van Jaarsveld, C. H. M., Potts, H. W. W., & Wardle, J. (2010). How are habits formed: Modelling habit formation in the real world. European Journal of Social Psychology, 40(6), 998-1009. https://doi.org/10.1002/ejsp.674
Lorenz, T., Beer, C., Pütz, J., & Heinitz, K. (2016). Measuring psychological capital: Construction and validation of the compound PsyCap scale (CPC-12). PloS one, 11(4), e0152892. https://doi.org/10.1371/journal.pone.0152892
Lupșa, D., Vîrga, D., Maricuțoiu, L. P., & Rusu, A. (2020). Increasing psychological capital: A pre‐registered meta‐analysis of controlled interventions. Applied Psychology, 69(4), 1506-1556. https://doi.org/10.1111/apps.12219
Luthans, B. C., Luthans, K. W., & Avey, J. B. (2014). Building the leaders of tomorrow: The development of academic psychological capital. Journal of Leadership & Organizational Studies, 21(2), 191-199. https://doi.org/10.1177/1548051813517003
Luthans, F., Avey, J. B., Avolio, B. J., & Peterson, S. J. (2010). The development and resulting performance impact of positive psychological capital. Human Resource Development Quarterly, 21(1), 41-67. https://doi.org/10.1002/hrdq.20034
Luthans, F., Avey, J. B., Avolio, B. J., Norman, S. M., & Combs, G. M. (2006). Psychological capital development: Toward a micro‐intervention. Journal of Organizational Behavior, 27(3), 387-393. https://doi.org/10.1002/job.373
Luthans, F., Avolio, B. J., Avey, J. B., & Norman, S. M. (2007). Positive psychological capital: Measurement and relationship with performance and satisfaction. Personnel Psychology, 60(3), 541-572. https://doi.org/10.1111/j.1744-6570.2007.00083.x
Luthans, F., Luthans, K. W., & Luthans, B. C. (2004). Positive psychological capital: Beyond human and social capital. Business Horizons, 47(1), 45-50. https://doi.org/10.1016/j.bushor.2003.11.007
Luthans, F., Youssef-Morgan, C. M., & Avolio, B. J. (2015). Psychological capital and beyond. Oxford University Press.
Martin, A., Sanderson, K., Scott, J., & Brough, P. (2009). Promoting mental health in small-medium enterprises: An evaluation of the “Business in Mind” program. BMC Public Health, 9, 239. https://doi.org/10.1186/1471-2458-9-239
Masten, A. S., & Reed, M. G. J. (2002). Resilience in development. In C. R. Snyder & S. J. Lopez (Eds.), Handbook of positive psychology (pp. 74-88). Oxford University Press.
Matos, M. G. (2017). Sem medo e sem riscos: Desafios da psicologia na prevenção e promoção do século 21. In Ordem dos Psicólogos Portugueses (Ed.), Pensar a Psicologia (pp. 50-65). https://www.ordemdospsicologos.pt/ficheiros/documentos/pensar_a_psicologia_ebook.pdf
Nepomuceno, A., & Conceição, J. (2020). Técnica 02: Tomando Decisões. In J. Conceição & G. Bueno (Eds.), 101 técnicas da terapia cognitivo-comportamental (pp. 14). UNC.
Nunes, A. P. L. (2017). Programa de intervenção para prevenção do burnout em unidades de cuidados intensivos: Um dever ético (Doctoral Dissertation, Universidade Católica Portuguesa). Repositorio Universidade Católica Portuguesa. http://hdl.handle.net/10400.14/24180
Paulitisky, E. E., & Conceição, J. (2020). Técnica 20: Reformulação de Imagens Mentais. In J. Conceição & G. Bueno (Eds.), 101 técnicas da terapia cognitivo-comportamental (pp. 44-45). UNC.
Read, M. (2024, 1st October). How to measure employee wellness programs ROI in 2025. Forma. https://www.joinforma.com/resources/employee-wellness-programs-roi
Rodrigues, F. J. S. (2022). O capital psicológico positivo como preditor do bem-estar no trabalho: Um estudo no setor do retalho (Master's thesis, Universidade de Lisboa). Repositório Científico de Acesso Aberto da ULisboa. http://hdl.handle.net/10400.5/27235
Rodrigues, M. C. H., & Conceição, J. (2020). Técnica 69: Meditação de Um Minuto. In J. Conceição & G. Bueno (Eds.), 101 técnicas da terapia cognitivo-comportamental (pp. 120-121). UNC.
Rudey, C. W. O., & Conceição, J. (2020). Técnica 08: Role-Play Racional-Emocional. In J. Conceição & G. Bueno (Eds.), 101 técnicas da terapia cognitivo-comportamental (pp. 22). UNC.
Ruiz, A. P. P. S., Viseu, J. N. R., Cifuentes-Tinjaca, C. D. & Jesus, S. N. (2024). Positive psychological capital in health professionals: A systematic literature review. Revista Latinoamericana de Psicología, 56, 164-179. https://doi.org/10.14349/rlp.2024.v56.17
Ruiz, A. P. P. S., Viseu, J. N. R., Cifuentes-Tinjaca, C. D. & Jesus, S. N. (2025). Interventions to Foster PsyCap: A Systematic Literature Review (Unpublished manuscript).
Russo, S. D., & Stoykova, P. (2015). Psychological capital intervention (PCI): A replication and extension. Human Resource Development Quarterly, 26(3), 329-347. https://doi.org/10.1002/hrdq.21212
Sachweh, E. S., & Conceição, J. (2020). Técnica 16: Roda da Vida. In J. Conceição & G. Bueno (Eds.), 101 técnicas da terapia cognitivo-comportamental (pp. 35-38). UNC.
Salanova, M., & Ortega-Maldonado, A. (2019). Psychological capital development in organizations: An integrative review of evidence-based intervention programs. In L. E. van Zyl & S. Rothmann (Eds.), Positive Psychological Intervention Design and Protocols for Multi-cultural Contexts (pp. 81-102). Springer. https://doi.org/10.1007/978-3-030-20020-6_4
Santos, A. A. D. C. (2021). O estado da arte do capital psicológico (psycap) grupal: uma revisão bibliométrica (Master's thesis, Universidade de Coimbra). Repositorio da Universidade de Coimbra. https://hdl.handle.net/10316/96523
Santos, M. C., & Wechsler, S. M. (2015). Análise das publicações científicas sobre otimismo em saúde no último triênio. Psicologia Argumento, 33(83). https://doi.org/10.7213/psicol.argum.33.083.AO03
Santos, N. R., Pais, L., Mónico, L. S., & Macedo, R. C. (2019). Capital psicológico: um estudo sobre o significado das suas dimensões. In L. Mónico, C. Carvalho, D. Dias, & P. Parreira (Eds.), Capital Psicológico, Estratégia e Gestão na Diversidade das Organizações (pp. 51-72). Escola Superior de Enfermagem de Coimbra.
Schaufeli, W., & Bakker, A. (2003). Utrecht work engagement scale: Preliminary manual. Occupational Health Psychology Unit, Utrecht University.
Scheier, M. F., & Carver, C. S. (1985). Optimism, coping, and health: assessment and implications of generalized outcome expectancies. Health Psychology, 4(3), 219-247. https://doi.org/10.1037//0278-6133.4.3.219
Secosan, I., Virga, D., Crainiceanu, Z. P., Bratu, L. M., & Bratu, T. (2021). The moderating role of personal resources between demands and Ill-Being of romanian healthcare professionals in the COVID-19 Pandemic. Frontiers in Public Health, 9, 2148. https://doi.org/10.3389/fpubh.2021.736099
Seligman, M. (2012). A vida que floresce: Um novo conceito visionário da felicidade e do bem-estar. Estrela Polar.
Sharp, R. (2019). Career crescendo: An experimental analysis of a 6-week work-site intervention to determine the developmental capacity of psychological capital. Journal of Management Development, 38(9), 719-732. https://doi.org/10.1108/JMD-10-2018-0295
Snyder, C. R., Irving, L. M., & Anderson, J. R. (1991). Hope and health. In C. R. Snyder & D. R. Forsyth (Eds.), Handbook of social and clinical psychology: The health perspective (pp. 285-305). Pergamon Pres.
Souza, M. F., da Costa Sousa, I., Vidal, E. C. F., & Vidal, E. C. F. (2015). Fatores contributivos para motivação dos profissionais de saúde da atenção básica de saúde. Caderno de Cultura e Ciência, Cariri, 13(2). https://doi.org/10.14295/cad.cult.cienc.v13i2.863
Stratman, J. L., & Youssef-Morgan, C. M. (2019). Can positivity promote safety? Psychological capital development combats cynicism and unsafe behavior. Safety Science, 116, 13-25. https://doi.org/10.1016/j.ssci.2019.02.031
United Nations. (2020). Sustainable Development Goals. http://www.un.org/sustainabledevelopment/sustainable-development-goals/
Viseu, J. N. R. (2017). A motivação profissional dos docentes do ensino básico e secundário: A influência de variáveis organizacionais, individuais e pertencentes à interface sujeito-organização (Doctoral dissertation, Universidade do Algarve). Repositório da Universidade do Algarve
World Health Organization. (2010). Ambientes de trabalho saudáveis: Um modelo para ação: Para empregadores, trabalhadores, formuladores de política e profissionais. https://apps.who.int/iris/bitstream/handle/10665/44307/9789241599313_por.pdf?sequence=2&isAllowed=y
World Health Organization. (2020). Global Plan of Action on Workers’ Health 2008–2017.
Yang, S., Huang, H., Qiu, T., Tian, F., Gu, Z., Gao, X., & Wu, H. (2020). Psychological capital mediates the association between perceived organizational support and work engagement among Chinese doctors. Frontiers in Public Health, 8, 149. https://doi.org/10.3389/fpubh.2020.00149
Youssef‐Morgan, C. M., & A. Sundermann, D. (2014). Positive interventions: from prevention to amplification. In T. W. Taris, M. C. W. Peeters & J. de Jonge (Eds.), An introduction to contemporary work psychology (pp. 458-480). John Wiley & Sons. https://doi.org/10.1002/9781394259564.ch19
Youssef-Morgan, C. M., & Luthans, F. (2011). Psychological capital: Meaning, findings, and future directions. In G. M. Spreitzer & K. S. Cameron (Eds.), The Oxford handbook of positive organizational scholarship (pp. 16-27). Oxford University Press. https://doi.org/10.1093/oxfordhb/9780199734610.013.0002
Zeng, L., Feng, F., Jin, M., Xie, W., Li, X., Li, L., Peng, Y., & Wang, J. (2023). Psychological capital and organizational citizenship behavior among nurses during the COVID-19 epidemic: mediation of organizational commitment. BMC Nursing, 22(1), 172. https://doi.org/10.1186/s12912-023-01332-7
Funding: This study did not receive any external funding or financial support.
Conflict of interest: The authors declare that they have no conflicts of interest.
How to cite: Ruiz, A. P. P. S., Viseu, J. N. R., Cifuentes Tinjaca, C. D., & Jesus, S. N. (2026). PsyCap Promotion Intervention Program (PIPP) for Healthcare Professionals: Intervention Description. Ciencias Psicológicas, 20(1), e-4584. https://doi.org/10.22235/cp.v20i1.4584
Authors’ contribution (CRediT Taxonomy): 1. Conceptualization; 2. Data curation; 3. Formal Analysis; 4. Funding acquisition; 5. Investigation; 6. Methodology; 7. Project administration; 8. Resources; 9. Software; 10. Supervision; 11. Validation; 12. Visualization; 13. Writing: original draft; 14. Writing: review & editing.
A. P. P. S. R. has contributed in 1, 2, 3, 5, 6, 7, 8, 9, 11, 12, 13, 14; J. N. R. V. in 3, 10, 11, 14; C. D. C.-T. in 3, 10, 11, 12; S. N. de J. in 3, 10, 11, 14.
Scientific editor in-charge: Dr. Cecilia Cracco.
Ciencias Psicológicas; v20(1)
January - June 2026
10.22235/cp.v20i1.4584